Prevention is better than cure, but if you happen to have sepsis, get to us in a timely manner. Don’t wait.
Dr. Mbonu Ikezuagu, Vice President and Chief Quality Officer, ThedaCare
You’re probably familiar with what it feels like to have your body fight an infection. When a bacteria or virus infiltrates, your body kicks into high gear to overcome the infection.
You may develop a fever. While that’s often uncomfortable, it’s part of the body doing its job to fight infection.
Sepsis is a different matter. It’s the body’s overwhelming and life-threatening response to infection, according to the Sepsis Alliance. Sepsis is a medical emergency that requires rapid diagnosis and treatment. The condition can lead to severe sepsis and septic shock. It can also cause tissue damage, organ failure, and death.
Mbonu Ikezuagu, MD, Vice President and Chief Quality Officer for ThedaCare, describes sepsis another way.
“It’s like you’re in a war zone, trying to kill the enemy around you. You set off a bomb but end up destroying your own people in the process,” he says. “That’s exactly what your body is doing: trying to kill the bacteria, but you end up harming your body in the process.”
Heavy Toll
Sepsis is costly both in terms of the lives it claims and dollars devoted to treating the condition. It’s the No. 1 cost of hospitalization in the United States. Sepsis costs U.S. health care systems approximately $62 billion annually. This is only a portion of all sepsis-related costs, since many people face additional costs after discharge, according to the Sepsis Alliance.
We mark Sepsis Survivor Week every February and Sepsis Awareness Month each September. These observances provide an opportunity learn key facts about this potentially life-threatening condition.
Five Points to Understand About Sepsis
1. Anyone can develop sepsis, but certain populations are at greater risk.
Those include people 65 and older, children younger than 1, those with chronic conditions, and individuals with weakened immune system, according to the Centers for Disease Control and Prevention.
Conditions that put people at risk include diabetes, cancer, kidney disease, lung conditions such as chronic obstructive pulmonary disease (COPD), and end-stage organ failure, such as liver or heart failure. Sepsis survivors and people who were recently hospitalized or experienced severe illness also are at greater risk.
2. Take steps to avoid developing sepsis.
- Manage chronic conditions
- Wash your hands frequently
- Keep cuts clean and covered until they’re healed
- Wear a mask in crowded places if you have compromised immunity
- Stay on top of vaccines
3. Any type of infection can lead to sepsis.
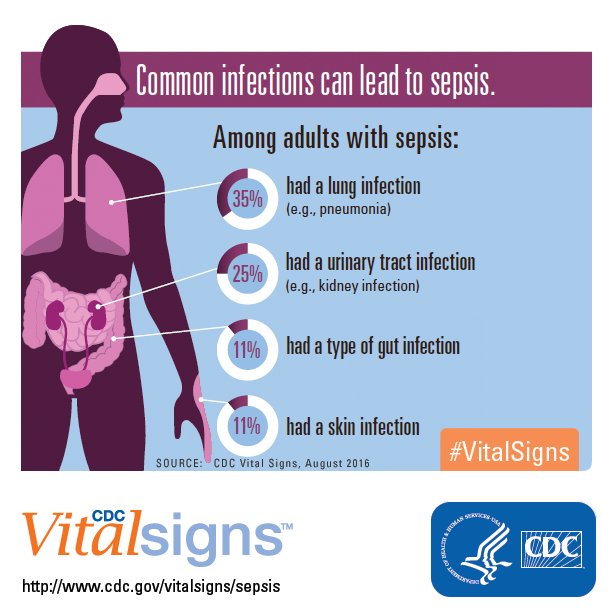
This includes bacterial, viral, or fungal infections. Common infections within the body can lead to sepsis. These include infections affecting the:
- Lungs, such as pneumonia
- Bladder — urinary tract infection or pyelonephritis and other parts of the urinary system
- Skin — cellulitis or wound infection
- Digestive system — infection in the gut
4. Know the symptoms.
Sepsis symptoms:
- Change in mental status
- Fast, shallow breathing
- Sweating for no clear reason
- Feeling lightheaded
- Fever or low body temperature
- Shivering
- Symptoms specific to the type of infection, such as painful urination from a urinary tract infection or worsening cough from pneumonia
Septic shock symptoms:
- Inability to stand up
- Strong sleepiness or difficulty staying awake
- Major change in mental status, such as extreme confusion
5. Act quickly if you suspect sepsis.
“The majority of our community is coming in to us late,” Dr. Ikezuagu says. “By the time they come in, we have the medicines, we have everything, but it’s sometimes too late to intervene.”
Where you seek care depends on your symptoms. Sepsis shares symptoms common with other conditions, so it’s important to look at all the symptoms and risk factors together, Dr. Ikezuagu says. If you have milder symptoms, you can call your primary care provider’s office or visit an urgent or walk-in care site.
If you’re experiencing severe symptoms, including difficulty breathing, extreme lethargy, and an altered mental state, call 911 or go to the emergency department.

Early, thorough treatment with medication and other interventions raises the likelihood of recovery. With increased awareness around sepsis, Dr. Ikezuagu hopes to see better outcomes.
“Prevention is better than cure, but if you happen to have sepsis, get to us in a timely manner. Don’t wait,” he says.

